If you are receiving Medicaid benefits in Arizona through Arizona’s Medicaid Agency, the Arizona Health Care Cost Containment System (AHCCCS), every 12 months you must renew your eligibility to continue to receive AHCCCS benefits. This is known as “Medicaid redetermination.”
In this post, we cover the Medicaid redetermination process for AHCCCS in Arizona.
If you are currently enrolled under AHCCCS coverage, or you have questions about eligibility for AHCCCS health plan coverage, including coverage for child dental services, call the Kids Dental Office of Phoenix at (602) 903-4894 or contact us online.
What is AHCCCS Coverage in Arizona?
AHCCCS is the Arizona partner program that provides federal Medicaid benefits to residents in the state from eligible households.
Eligibility determinations are based on household modified adjusted gross income, family size, and your citizenship status. For eligible low-income families, AHCCCS covers the cost of necessary children’s healthcare, including dental care, for children under 19 years of age.
AHCCCS coverage is not permanent and must be renewed every 12 months to reevaluate your eligibility and continue receiving benefits.
What is the Medicaid Redetermination Process in Arizona?
Your renewal for Medicaid coverage eligibility occurs every 12 months. About 60 days before the end of the 12th month, AHCCCS will evaluate your eligibility using data from your prior application. Then AHCCCS will obtain electronic data from Federal and State sources and use this information to make its own eligibility determination.
If you are still eligible, AHCCCS will send you an approval letter. These renewals are known as No Response Renewals and are completed automatically.
If eligibility cannot be determined using available data or the information indicates that you are no longer eligible, then you must provide the information needed to complete the renewal process.
In this situation, you will be sent a pre-populated renewal form along with a Request for Information letter that outlines the necessary information to complete the renewal. This is known as Response Required Renewal.
In this case, you should receive a redetermination notice from AHCCCS 90 days before your coverage expires. The notice will inform you of your renewal deadline and includes instructions on how to renew your Medicaid coverage.
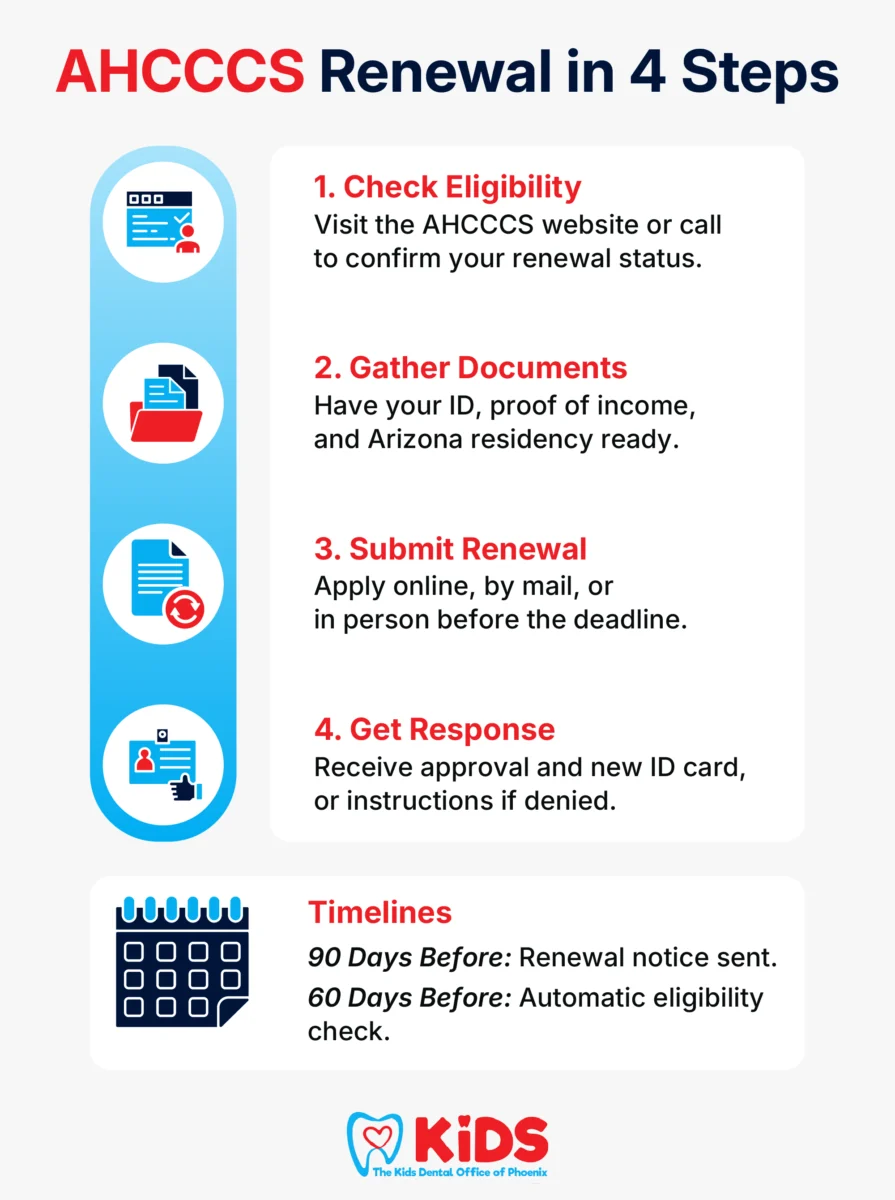
Once you receive your redetermination notice from AHCCCS, you will need to complete the following steps:
- Check your eligibility status. To check your Medicaid eligibility, visit the AHCCCS website or call the AHCCCS customer service hotline. The website and hotline will provide information on how to apply for Medicaid, your eligibility requirements, and other related resources.
- Gather necessary documentation. You will need to have the required documents to support your redetermination claim. These may include identification, proof of income, and proof of Arizona residency.
- Complete and submit the renewal application. You can apply for AHCCCS renewal online, by mail, or in person at your local AHCCCS office. The renewal application will ask for updated information about your household and income. After completing the renewal application, submit it before the deadline stated in your renewal notice.
- Wait for a response. Once you have submitted your renewal application, you will need to wait for a response from AHCCCS. If your application is approved, you will receive a new Medicaid ID card. If your application is denied, AHCCCS will provide information on how to appeal the decision.
If you do not provide the requested information by the due date, your eligibility will stop. If you send the requested information, AHCCCS will decide if you are eligible to renew.
If you no longer meet the eligibility criteria for AHCCCS, you will be screened for possible eligibility for other programs. Ultimately, you will receive either an approval letter or a discontinuance letter.
Other Options if You No Longer Qualify for Medicaid in Arizona
If your household no longer qualifies for AHCCCS, other healthcare options are available to help cover the costs of your children’s healthcare and dental care.
KidsCare
For example, KidsCare is the program Arizona has to provide federally subsidized health insurance for children under the Children’s Health Insurance Program (CHIP). KidsCare provides health coverage to children whose families have incomes too high to qualify for Medicaid coverage under the Arizona Health Care Cost Containment System (AHCCCS) but who still cannot afford private health insurance coverage.
Unlike AHCCCS coverage, which is premium-free, those who qualify for KidsCare are subject to monthly premiums.
Subsidized Health Insurance Options
Another option is to purchase subsidized health insurance under the Affordable Care Act through the federal Health Insurance Marketplace or eHealth. These offer a variety of health insurance marketplace plans based on your income and family size.
Do You Have Questions About AHCCCS Eligibility for Your Child’s Dental Services?
At the Kids Dental Office of Phoenix, we accept Medicaid and CHIP insurance payments for dental and orthodontic services for children. We can help you know if your household is eligible for Medicaid or CHIP coverage in Arizona, including whether your family is eligible for Medicaid renewal.
To learn more, call us at (602) 903-4894 or use our contact form to ask a question or schedule an appointment for your child.
With Medicaid or CHIP coverage available for children through age 18, you can afford to have the best dental care possible for your children.
